An accurate diagnosis of the type of leukemia is important. The exact diagnosis helps the doctor to estimate how the disease will progress and determine the appropriate treatment
Diagnosing acute myeloid leukemia (AML) and your AML subtype usually involves a series of tests. Some of these tests may be repeated during and after therapy to measure the effects of treatment.
Tests Your Doctor May Use to Diagnose AML
Blood and bone marrow tests are used to diagnose AML and the AML subtype. A change in the number and appearance of blood cells helps to make the diagnosis.
Blood Tests
A complete blood count (CBC) with differential counts the number of red cells, white cells and platelets in the blood. The CBC should include a differential, which measures the numbers of the different types of white blood cells in the sample. People with AML often have a high number of white blood cells, but most of these are leukemia (blast) cells that do not protect against infection. They may also have a low number of red blood cells and platelets.
Bone Marrow Tests
Samples of marrow cells are obtained by bone marrow aspiration and biopsy. Bone marrow testing involves two steps usually performed at the same time in a doctor's office or a hospital:
- A bone marrow aspiration to remove a liquid marrow sample
- A bone marrow biopsy to remove a small amount of bone filled with marrow
Bone marrow samples are usually taken from the hip bone. Both samples are examined under a microscope to look for chromosomal and other cell changes.
Cell Examination
At the laboratory, a hematopathologist examines the blood and bone marrow samples. This is a type of doctor who has special training in identifying blood diseases by studying cells under a microscope and performing other specialized tests on these blood cells.
Immunophenotyping (Flow Cytometry)
This test can diagnose specific types of leukemia and lymphoma by detecting certain proteins on a cell's surface. The sample of cells comes from a blood or bone marrow test. The test can also be used to see if there are any cancer cells remaining in the body after treatment called "minimal/measurable residual disease (MRD)."
Cytogenetic Analysis (Karyotyping)
This test uses a microscope to examine the chromosomes inside the cells. Chromosomes are the part of a cell that contains genetic information. Normal human cells contain 23 pairs of chromosomes, for a total of 46 chromosomes. The chromosomes are a certain size, shape and structure. In some cases of AML, the chromosomes of the leukemia cells have abnormal changes.
Cytogenetic testing is done with either a bone marrow or blood sample. The leukemia cells are allowed to grow in a laboratory and then stained. The sample is then examined to see the arrangement of the chromosomes, called a “karyotype.” The karyotype shows if there are any abnormal changes in the leukemia cells. In some cases, this provides important information to determine treatment options and prognosis.
Fluorescence In Situ Hybridization (FISH)
This very sensitive test is used to examine genes or chromosomes in cells and tissues. Doctors use FISH to detect certain abnormal changes in the chromosomes and genes of leukemia cells. Pieces of DNA that contain special fluorescent dyes are prepared in the laboratory and added to the leukemia cells on a glass slide. The pieces of DNA that bind to certain genes or areas of chromosomes light up when the slide is viewed under a specialized “fluorescence” microscope. Not only can FISH identify most abnormal changes that can be seen with karyotype testing under a microscope, but it can also detect some changes that are too small to be seen with karyotype testing. It is not, however, used as a general screening tool. FISH has one disadvantage—before the test is performed, the doctor must select the specific chromosomes or genes that are going to be examined.
Polymerase Chain Reaction (PCR)
This is a very sensitive test that finds and measures genetic mutations and chromosome changes that are too small to be seen with other tests or even with a powerful microscope. PCR can find a single leukemia cell in approximately 100,000 normal cells. This test is given during treatment or after treatment, and the results allow doctors to determine the amount of minimal/measurable residual disease (MRD), the small number of cancer cells left in the body after treatment.
Biomarker Testing
Biomarker testing, also called “molecular testing” or “genomic testing” refers to a number of different laboratory tests that examine the exact sequence (order) of DNA or RNA. This makes it possible to identify a variety of genetic changes in a patient’s cancer cells. These changes are important in guiding risk assessment and prognosis and may also inform treatment decisions. The information it provides can help doctors to determine which patients are at high risk and may need more intensive treatment or may benefit from treatment with novel therapies.
There are targeted sequencing tests (also called “multigene panels”) that look for specific mutations in the cancer cells. These tests focus on specific sets of genes or areas of DNA. There are also broad DNA sequencing tests (genomic screening tests) that analyze the sequence of large regions of DNA, rather than looking for mutations of specific genes. Doctors may also order sequencing of all the DNA in your entire genome. This test is known as “whole genome sequencing.”
The term “next-generation sequencing (NGS)” is a catch-all term used to describe a number of different modern sequencing technologies. These technologies allow for sequencing of DNA and RNA much more quickly and cheaply than sequencing methods that were used previously.
Since the introduction of DNA sequencing, the number of mutated genes that can be detected in AML patients has increased considerably. These markers are important in guiding risk assessment and prognosis and are also used to guide treatment decisions.
Generally, biomarker testing should be done when the cancer is first diagnosed and again after a relapse. This is because patients may acquire additional genetic abnormalities after they complete their initial, “first-line” treatment.
Pre-Treatment Tests
Before you start treatment, you doctor will perform tests to learn more about your overall health and your disease, including:
- Blood chemistry profile
- Human leukocyte antigen (HLA) typing
- An HLA test is done before allogeneic stem cell transplantation to find out if there is a tissue match between a potential donor and the patient receiving the transplant.
- Heart tests
Diagnosing AML
Your doctor will work with a hematopathologist to confirm the diagnosis. For a person to be diagnosed with AML, generally 20 percent or more of the cells in the bone marrow or blood must be myeloblasts.
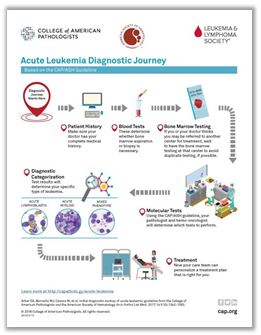
This infographic describes the steps doctors take to diagnose AML:
Click here for the steps involved with a new diagnosis of acute leukemia.
Chromosome and Gene Abnormalities
Chromosomal changes and genetic mutations are an important prognostic factor for predicting remission rates, relapse risks and survival outcomes. However, not all patients have a chromosomal abnormality, and patients may have different gene mutations from other AML patients. Your doctor will perform a molecular analysis on your cells to identify specific genetic changes. See the LLS fact sheet, Cancer Molecular Profiling for more information.
Newly Diagnosed Checklist
The College of American Pathologists (CAP) and the American Society of Hematology (ASH) provide practical guidance for patients and caregivers coping with a new diagnosis of acute leukemia. This checklist will help ensure that you receive the best treatment for your unique situation.
Related Links
- Download or order The Leukemia & Lymphoma Society's free booklet, Acute Myeloid Leukemia in Adults.
- Blood Tests
- Understanding Blood Counts
- Bone Marrow Tests
- Questions and Answers for Patients With Acute Leukemia