- Largest study to date to report detailed findings by blood cancer and treatment type
- Non-Hodgkin lymphoma patients less likely to have detectable antibodies
- Among leukemia patients, those with chronic lymphocytic leukemia most likely to be seronegative
- Multiple myeloma patients had higher rates of antibodies compared to other blood cancers
- LLS experts say vaccination offers protection to most blood cancer patient and should be combined with prevention precautions for best protection
RYE BROOK, N.Y., July 22, 2021 – About one in four blood cancer patients fail to produce detectable antibodies after COVID-19 vaccination, but results vary substantially by type of blood cancer, according to a new study from The Leukemia & Lymphoma Society (LLS) that was published today in the journal Cancer Cell (see full paper and tables). While earlier studies, as well as three others that appear alongside the LLS study today in Cancer Cell,1-3 have shown that certain blood cancer patients may not get optimal protection from vaccination, the LLS study is the largest to date examining over 1,400 patients and the first to provide a detailed look across all the major blood cancer and treatment types.
“Although some patients with hematologic malignancies will not mount a full antibody response compared to healthy individuals, vaccines are safe and offer protection to the majority of blood cancer patients,” said Dr. Gwen Nichols, Chief Medical Officer at LLS. “But not everyone will be protected, and blood cancer patients are at increased risk of serious illness and death from COVID-19. We encourage blood cancer patients to take every measure to protect themselves from COVID-19 by getting vaccinated and continuing to take preventative precautions. This includes wearing a mask, social distancing, and avoiding crowds and poorly ventilated indoor spaces.”
LLS estimates that nearly 250,000 blood cancer patients in the U.S. will not have detectable antibodies following COVID-19 vaccination. Dr. Nichols and LLS also stress that when others get vaccinated, they are not only protecting themselves, but are helping to protect these patients and the millions of others in the U.S. with suppressed immune systems.
The study (NCT04794387) was made possible by the more than 8,000 current and former blood cancer patients who became citizen scientists and joined the LLS National Patient Registry, a project of the Michael J. Garil Patient Data Collective. This research registry is a collaboration between LLS and the consumer healthcare technology company Ciitizen, whose patient-mediated medical records platform powered this research. All participating patients consented to share their de-identified medical data through the Ciitizen platform.
Today’s study reports on 1,445 registry participants who had their antibodies measured at least two weeks after their second dose of either the Moderna or Pfizer mRNA vaccine. These vaccines were by far the most commonly used during the March 12 to May 5, 2021 period covered by this study. LLS is conducting ongoing studies among Registry participants and expects to report additional data in 2021.
Seronegative rates vary by blood cancer type and treatment
Non-Hodgkin lymphoma patients are less likely to have detectable antibodies. The percentage of patients with non-Hodgkin lymphoma who were seronegative following vaccination ranged from 21% to 56%. This includes patients with diffuse large B cell, mantle cell, marginal zone and follicular lymphomas, as well as Waldenstrom’s macroglobulinemia. In contrast, just one of 64 Hodgkin lymphoma patients was seronegative. Many of these patients were treated with anti-CD20 antibodies such as rituximab, which eliminates B-cells that make antibodies.
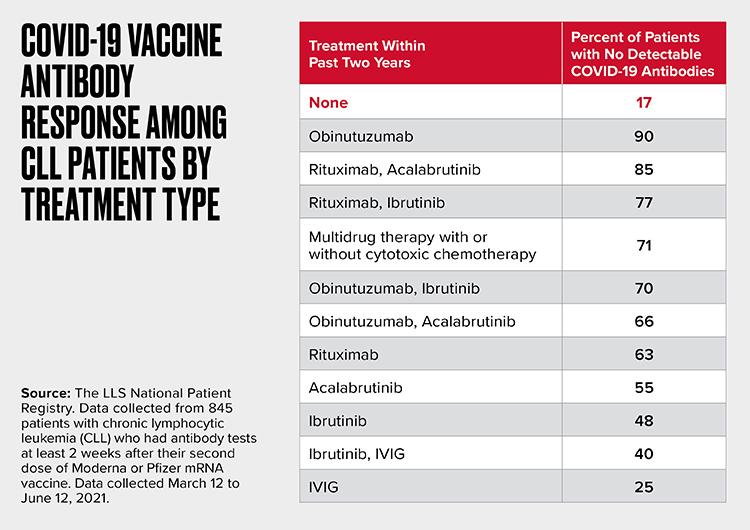
Among leukemia patients, those with chronic lymphocytic leukemia (CLL) are most likely to be seronegative. More than one-third (36%) of patients with CLL, the most common leukemia in U.S. adults, were seronegative after vaccination. Nearly three in 10 of them had no cancer therapy in the past two years, showing that the disease itself may impair the B cell function needed to make antibodies to vaccines.
However, the seronegative rates were even higher in CLL patients who were treated within the last two years with drugs that impair B-cells, including BTK inhibitors such as ibrutinib, anti-CD20 antibodies or combinations of these therapies or their use with venetoclax, a BCL2 inhibitor.
Multiple myeloma patients had higher rates of detectable antibodies compared to other blood cancers: Only 5% of patient with multiple myeloma were seronegative. Other studies have reported higher seronegative rates (up to 15%) in multiple myeloma patients.
Groundbreaking CAR T-cell immunotherapy may impact vaccine response: The study examined the impact of CAR T-therapy, which harnesses the body’s T-cells to fight cancer, on vaccine response. Six of seven patients who received CAR-T for CLL, diffuse large B cell or follicular lymphoma were seronegative after vaccination. These low response rates are similar to another study also reported in Cancer Cell1 and likely due to elimination of normal B-cells by the therapy. In contrast, four of five patients who received a different type of CAR-T for multiple myeloma produced robust antibodies. The registry is actively seeking additional CAR-T patients to increase the strength of its data.
Larry Saltzman, a physician who leads the LLS National Patient Registry and long-time CLL patient himself has been treated extensively with B-cell depleting therapies including CAR-T. “LLS’s leadership in cancer research was instrumental in the development of drugs that have literally saved my life. While we all want to go back to our pre-pandemic lives, that would be a big mistake for me. I chose to get vaccinated as soon as the vaccine was available to me, and I continue to mask up and take other precautions to make sure I’m here for my family, including my grandchildren.”
LLS experts urge patients to take precautions and follow vaccine recommendations
LLS receives calls from patients every day trying to understand their risk of COVID-19 and how protected they are from vaccination. Dr. Nichols urges patients to talk with their doctors, get vaccinated, continue to take preventative precautions, and to enroll in clinical trials, if possible, to help find more answers.
The Centers for Disease Control and Prevention (CDC) recently provided interim guidance for fully vaccinated immunocompromised individuals acknowledging that they should be should be counseled about the potential for reduced immune responses to COVID-19 vaccines and the need to continue to follow current prevention measures. The CDC will also be discussing the possibility of recommending booster doses for patients with compromised immune systems, including blood cancer patients today. Emerging data in two studies examining the response in seronegative solid organ transplant patients, as well as a single blood cancer patient, have reported an increase in antibody production after being given a booster shot following full dosing of the SARS-CoV-2 vaccines.4-6
Dr. Nichols says LLS is supporting trials to help answer questions about booster shot safety. “Because we need to understand if this is safe and effective, it is important for patients to enroll in a clinical trial rather than getting boosters on their own,” she says. She also cautions that anyone getting a third dose at this time should continue to take other precautions until we learn more.
With the Delta variant emerging and a large portion of the population still unvaccinated in pockets of the country, Dr. Nichols urges blood cancer patients to remain vigilant and to see their doctor immediately if they have been exposed to anyone with COVID. “It is imperative that blood cancer patients see a doctor immediately if they’ve been exposed to COVID,” says Nichols. “Patients who test positive can receive treatments such as antibody cocktails that may help prevent them from getting sick.”
If you are a blood cancer patient or survivor, read more in our COVID-19 vaccine FAQ here. If you have questions about the LLS COVID-19 antibody research study, click here.
For more COVID-19 information, check out our Resource Page
References
- Thakkar A, et al. (2021) Cancer Call. doi: doi: 10.1016/j.ccell.2021.06.002. [Epub ahead of print].
- Van Oekelen O, et al. (2021) Cancer Cell. doi: 10.1016/j.ccell.2021.06.014. [Epub ahead of print].
- Addeo A, et al. (2021) Cancer Cell. doi: https://doi.org/10.1016/j.ccell.2021.06.009.[Epub ahead of print].
- Hill JA, et al. (2021) Cancer Cell. doi: https://doi.org/10.1016/j.ccell.2021.06.015. [Epub ahead of print].
- Werbel WA, et al. (2021) Ann Intern Med. doi: 10.7326/L21-0282.
- Kamar N, et al. (2021) N Engl J Med. doi: 10.1056/NEJMc2108861.
About the LLS National Patient Registry
The LLS National Patient Registry, a project of the Michael J. Garil Patient Data Collective, was created to honor the memory of Michael Garil, who was diagnosed with acute lymphoblastic leukemia in 1974 at the age of seven. His parents, Ethel and Bernard Garil have generously supported the creation of the LLS National Patient Registry to gather vital information from a large pool of people affected by blood cancers. The trial was conducted under IRB review with electronic consent of patients. Data were de-identified before being analyzed for vaccine results and all patient records are held in strict confidence.
Joining The LLS National Patient Registry today is safe and easy. Your participation will have a far-reaching impact on improving care for everyone with blood cancer. Visit LLS.org/Registry to learn more about the Registry and to sign up.
About The Leukemia & Lymphoma Society
The Leukemia & Lymphoma Society® (LLS) is a global leader in the fight against cancer. The LLS mission: Cure leukemia, lymphoma, Hodgkin's disease and myeloma. LLS funds lifesaving blood cancer research around the world, provides free information and support services, and is the voice for all blood cancer patients seeking access to quality, affordable, coordinated care.
Founded in 1949 and headquartered in Rye Brook, NY, LLS has regional offices throughout the United States and Canada. To learn more, visit www.LLS.org. Patients should contact the LLS Information Resource Center at (800) 955-4572, Monday through Friday, 9 a.m. to 9 p.m., ET.
For additional information visit lls.org/lls-newsnetwork. Follow us on Facebook, Twitter, and Instagram.
About Ciitizen
Ciitizen is a leading, patient-mediated online platform which allows patients to securely collect, organize and maintain their medical records. Ciitizen turns these medical records into structured, longitudinal data that can be shared by patients with whomever they want - including for their own clinical treatment or for observational research. As a patient-directed care platform, Ciitizen believes patients should have full control of directing the use of their data, which serves as one of the richest sources of real-world evidence, unlocking new options for patients and the community. To learn more, visit www.ciitizen.com/LLS or email [email protected].
Contact:
Irene Tung
Senior Manager, Mission Communications
The Leukemia & Lymphoma Society
[email protected]
(718)-414-7910